Please read the updated version of this article HERE

Recently a case study was reported, where a doctor and a nurse at a clinic used a cocktail of medications to enable a transwoman to fulfill his goal to breastfeed his adopted infant.
In this article, I will refer to their patient as “trans-identified male” and “he” because there are few fields of medicine in which correctly identifying patient’s sex is more pertinent than in pregnancy, birth and breastfeeding.
As a doctor, I have multiple concerns regarding this study and this is my analysis.
The trans-identified male patient, who is referred to as a “she” throughout the study, “explained that her partner was pregnant but not interested in breastfeeding, and that she (the trans-identified male patient) hoped to take on the role of being the primary food source for her infant.”
There is no evidence that clinicians who conducted this experiment met with or interviewed the mother to confirm these claims or that they obtained informed consent from the mother by discussing possible risks that male drug-induced nipple discharge could pose to the infant.
The trans-identified male patient was reported to have a medical history of “gender incongruence” but he hasn’t had any gender reassignment surgeries, which means that he was a fully sexed male. There was no other relevant medical history reported.
On presentation, the patient was on a gender-affirming regimen that included spironolactone (a heart medication used in this case as an androgen blocker), estradiol, micronised progesterone and “occasional” clonazepam and zolpidem for panic disorder and insomnia.
At initial appointment, the patient had gynaecomastia (abnormally enlarged breasts in a man, Tanner stage V) that was likely a side effect of spironolactone and cross-sex hormones he was taking.
Interestingly, it’s unclear what was the patient’s serum testosterone level, because two markedly different results were given, one in the body of text – 256 ng/dL – and another in the results table 1. – 20.52 ng/dL.


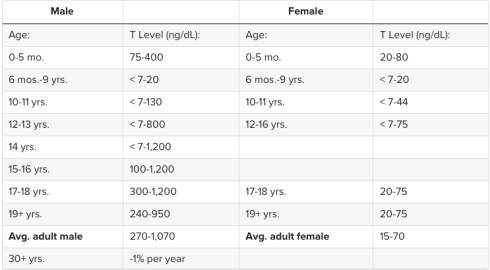
This is problematic not only because it constitutes a glaring inconsistency within the report, but also because the higher result indicates that the patient had male testosterone levels. Considering that the study reported no further testosterone data, indicating that they didn’t measure his testosterone level at any other point in the study, and that 75% of trans-identified men on spironolactone fail to reach testosterone level in the female range, and those who augment the treatment with estradiol have variable response, there is no reliable evidence that adequate androgen blockade was achieved, even though authors claimed that androgen blockade was an important part of the regimen.
What we do know, however, is that in mothers with PCOS (Polycycstic Ovary Syndrome), elevated testosterone levels inhibit breastfeeding while exposure of female foetuses to high maternal testosterone in the womb results in female infants having the same testosterone levels at birth as normal male infants.

This can cause medical complications such as precocious puberty, but also there’s evidence that such exposure is connected with gender non-conforming behaviour later in childhood.
Considering that gender non-conformance is currently an indication for diagnosing children as “transgender” and results in starting them on the highly experimental and potentially dangerous medical path to “gender reassignment”, which typically involves controversial treatment with puberty blockers and cross-sex hormones, the possible consequences need to be considered.

Because there are no studies proving absence of risk, there are ethical issues with enabling a man whose testosterone suppression isn’t adequately demonstrated, to breastfeed a potentially female infant.
And this brings us to another glaring omission in this report. While the authors consistently refer to the trans-identified male patient as “she”, they don’t state the sex of the infant involved in this experiment, revealing a worrying disinterest in the infant itself.
Clinicians also reported that their patient used domperidone, a drug that is banned in the US and is only used off-label internationally to induce lactation. Domperidone was sometimes used to treat reflux, but has been discontinued for use in children due to potential cardiac side-effects.
Even in countries where domperidone is given to mothers to stimulate lactation, it requires ensuring that the infant doesn’t have heart or liver abnormalities. There’s no evidence that clinic attempted to ascertain this.

Furthermore, there’s no evidence that the patient stopped using clonazepam , which can cause sedation in infants, or zolpidem (also known as Ambien), which could exacerbate effects of clonazepam, after the breastfeeding commenced.
When we talk about safety of drugs in breastfeeding, we weigh benefits of breastfeeding on health and bonding between mother and child, with risks of withdrawing medically necessary medicines mother might be taking.
Mothers who take medications that could be passed to their babies via breastmilk often decide not to breastfeed just so that they don’t risk affecting their baby’s health. Contrast this with a man who takes unnecessary medications, one of which is banned in the US, just so that he can fulfill his desire to breastfeed.
It’s worth mentioning that nipple discharge in men is always abnormal and a consequence of pathologically elevated prolactin due to certain medical conditions or a side effect of some medications.
There’s historical evidence of some men breastfeeding babies, eg. after wife’s death, but it was recognised that men’s milk was a poor substitute which, by maintaining hydration, may have helped infants survive in most adverse circumstances. We have no way of knowing but it is likely these men simply happened to have one of the abovementioned abnormalities,
Be as it may, following the regimen of medications and usage of a breast pump (as per stated protocol) the patient started to lactate, producing 8 oz of milk daily, and after the baby was born, he was reported to have been the sole source of this baby’s nurishment for 6 weeks.

Considering that a 5 lb baby needs about 12 oz of breastmilk, and more as their weight increases. 8 oz was clearly never enough, so authors’ claim that their patient managed to achieve the volume of milk that allowed him to be the sole source of nourishment for her child for 6 weeks is incorrect.
Furthermore, the authors’ claim that at 6 weeks, the patient began supplementing breastfeedings with 4–8 oz of Similac brand formula daily and they ressure us but give no evidence that “the child’s pediatrician reported that the child’s growth, feeding, and bowel habits were developmentally appropriate”.
This raises serious concerns about authenticity of the entire report. As far as can be ascertained from the study, authors never observed any breastfeeding nor did they meet the mother or the infant.
But let’s assume for the sake of the argument that somehow this case study was indeed based on real events, and that the infant survived for 6 weeks on 8oz of male drug-induced galactorrhea a day.
Mother’s breastmilk in context of pregnancy isn’t the same as drug-induced galactorrhea in a man, nor is breastmilk static in composition. It starts as colostrum (birth – 4 days) which is a thick fluid full of fat, vitamins and immunoglobulins. Then it changes to more calorific transitional milk (4 days – 2 weeks), which is high in fat and vitamins, and after that it becomes mature milk which is 90% water.
The authors of this study gave no indication that they analysed the content of this man’s nipple discharge, even though they talked at length about benefits of breastfeeding on mother and baby, none of which were applicable to their male patient or indeed the infant he allegedly fed.
Furthermore, mothers who don’t want to or are unable to breastfeed, are required to use baby formula, which closely approximates the nutritional content of mother’s milk at each stage, and are obliged to use it in adequate amounts. Why was their trans-identified male patient held to a drastically different standard of infant care?
Why didn’t this study explore reasons for this fully sexed male’s interest in breastfeeding a newborn? Considering that psychosexual disorders such as autogynaephilia are present in a proportion of typically fully sexed heterosexual males who identify as transwomen, this is an ethical issue.
There was also no mention of what kind of clinic this was. If this was an Obs&Gynae clinic, their primary responsibility was to the mother and child. If this was a transgender clinic, they had no business managing breastfeeding of an infant.
In my opinion, this study is an example of how transgender health clinics prioritise emotional needs of trans-identified males over the welfare of women and children and it is an unethical study, fraught with incomplete and misleading information, disingenuous analysis and undeclared conflict of interest.
Thank you for this excellent analysis.
Reading between the lines of this case report, it becomes clear that clinicians didn’t actually prescribe this (unethical) regimen. No responsible clinician would have prescribed for this unnecessary experiment. The patient obtained drugs online, and self-medicated.
This is one more example of transgender patients utilizing off-label drugs in experimental protocols, and getting clinicians to normalize it after the fact. (Often transgender clinicians, incidentally.)
Watch for this to show up in WPATH treatment standards within the next few years.
LikeLiked by 2 people
You are right Spryfield. I also see no evidence that any “breastfeeding” actually happened. Nobody witnessed it, or interviewed the mother. All they have is a word of their patient.
It would be in line with WPATH “research” to use this piece of medical fiction. I fear that frameworks for safeguarding children are being demolished.
https://www.thestranger.com/queer-issue-2017/2017/06/21/25225867/my-first-time-breastfeeding-my-daughter
LikeLiked by 1 person
This is absolutely disgusting that this man is poisoning that poor baby
LikeLike
This is the type of research ( and I Use the word research loosely) that will be used as evidence to further this perversion. The study is full of bias and constructed in an unscientific way. No matter, WPATH Will use it to further justifying this procedure with other transgender‘s.
LikeLike
Thank you for this detailed, excellent analysis.
One can only hope that this study is a fiction, for the sake of the child. But still it feeds the myth that men can do anything that women can – even the fundamentally female role of mothering.
LikeLiked by 2 people
Very well put Tricia. The study is exercise in male narcissim, delusion and total breakdown of safeguarding mechanisms for both the mother and the child. There’s a sinister undercurrent to transactivism that is using children for validation and sexual gratification of some trans-identified men, and even though paedophiles try to legalise their crimes every decade or so, it never stops being absolutely urgent to stop them. Case in point: https://www.thestranger.com/queer-issue-2017/2017/06/21/25225867/my-first-time-breastfeeding-my-daughter
It’s not an accident the fathers of post-modernism, Foucault and Derrida, and the fathers of transgenderism, Money, Kinsey, Benjamin, were all paedophile activists/apologists, or that WPATH is a rebranded Harry Benjamin International Gender Dysphoria Association (HBIGDA), or that this is being disseminated through queer theory, which is a brain child of post-modernism. But so many people aren’t aware of it, because the connections are not advertised and passive-aggressive male narratives are used to smear mothers and emotionally blackmail and gaslight general population and legislators, into, ultimately what, time will tell.
I believe any attempt at legislating child abuse will ultimately fail. The sociaty has shown firm distaste for it and it won’t be allowed. But even severely relaxed, or even holes in child safeguarding mechanisms ultimately benefit paedophile rings, who are, as we know, extremely well organised and often rooted in institutions which involve men with lots of resources in positions of power.
I am now carefully watching all developments that insinuate children 1) have a sexual orientation=sexual attraction=are sexual beings in adult sense, 2) are capable of consent regarding touching of their genitals (which puts onus on the child instead on adults to know what is and isn’t appropriate, and it completely compromises childcare of the most vulnerable infants and small children), 3) aim to alienate and separate children from their parents and 4) are normalising detailed discussions about a child’s genitals, bodies and sexual function. All three feature heavily in trans activism, from telling pre-pubescent “drag queens” that if their parents won’t allow them to be sexualised “they need new patents” to “so brave” news articles about “openly gay 3 year olds” that suggest the toddler is advertising their sexuality, most recent sinister position that parents need “infant’s consent” to change their nappies, to the tragic case dissected in the media via programme “I Am Jazz”.
https://www.advocate.com/youth/2017/6/05/meet-8-year-old-drag-queen-lactatia
https://www.lifesitenews.com/news/openly-gay-3-year-old-goes-viral-on-social-media
https://www.mirror.co.uk/news/world-news/im-going-change-your-nappy-12511101
http://www.thepublicdiscourse.com/2018/04/21220/
LikeLike
Very well done. I was disturbed, and yet had to roll my eyes, at this man talking about the ‘sexual excitement’ he got from ‘breastfeeding’ a child that isn’t even his. He has no biological connection to that child.
I found the men lactating bit interesting, but it’s clear men were not meant to lactate, as they do not gestate a child and cannot produce the regime required for them.
LikeLiked by 1 person
Thank you Reisen. Since I wrote this article, I became aware of another deeply worrying report. That these things are even happening, is evidence that safeguarding frameworks designed to protect children from abuse, are being dismantled. https://www.thestranger.com/queer-issue-2017/2017/06/21/25225867/my-first-time-breastfeeding-my-daughter
LikeLike
I wonder if it would work with a male who has klinefelter’s syndrome.
LikeLike
Men with Klinefelter syndrome are infertile, afaik, so they wouldn’t be the father, which would thank god rule out a whole demography here. I’ve also never heard that men with Klinefelter have higher occurrence of agp, although I’ve seen first hand that it can really mess with ones head to live with that condition, so in that sense I wouldn’t be surprised.
LikeLike
Men with Kleinfelter’s can father children using assisted reproduction techniques. But I agree, I never heard of a particular association between Kleinfelter’s and AGP.
LikeLike
Interesting how the word father is not being challenged as transphobic or exclusionary…. or is it, somewhere?
LikeLiked by 1 person
The BBC “reported” on this incident. They virtually reproduced the Press Release.
The Clinic is a PRIVATE trans clinic which states that if a trans individual has the money, they will try their hardest to accommodate your wishes. It is owned by a MtF trans nurse.
The clinic claimed to have had the patient’s permission to publish exerts from their case notes. As you say, no analysis was ever provided for the child so no one appears to have given consent for the CHILD’S medical details to be plastered all over the internet.
Even if we ignored all the inconsistencies and lack of due care, as you say the milk production was far below what was needed to sustain a baby, and the real mother was there on call who presumably was able to breastfeed.
So I made a formal complaint to the BBC. I stated that they had done zero investigation to ascertain if any of the claims were true. That the drug regime was in fact dangerous for a baby and the drugs could pass through the breastfeeding system and enter the baby’s system if it actually happened, which was a problem since the baby was, in fact, a boy. I said that the “report” was actually an “infomercial” because a Private Clinic that specifically looked to buy an outcome for patients had issued this Press Release to drum up business. And finally I said that the milk production would have seen the baby starve to death within days on account of it being far too low.
The BBC told me my complaint was nonsense and they were right to publish. When I tried to escalate it they wanted to limit my complaint to 50 words. When I refused to diminish it, and contacted the Executive directly I was told that I had pre-empted the complaint procedure and they could not consider it.
This is the utter contempt the BBC hold the health and well-being of babies in … but then we knew that after Saville, yeah?
LikeLiked by 3 people
Thank you for sharing this Tracy! BBC seems complicit in a very dangerous game…
LikeLiked by 3 people
I agree that it is disturbing there seems to be no care for the affect on the infant, and that it is unlikely this story is entirely true.
However, a couple of points stuck out to me: if a mother pumps only 8 ounces, it doesn’t mean she only produces that amount. Babies are so much more efficient than a pump. I mention this because a main reason women start to wean from breastfeeding is a belief that they are not making enough.
The other statement that disturbed me was that mothers are “required” to supplement with formula. There are other feeding options for babies including donor milk, and the mother should be the authority when making these decisions.
LikeLike
Thanks for your comment Sheila! Indeed you are right, there are other supplement options. I made a broad statement, as the supplementation with formula is the most common, and a baby couldn’t survive on 8oz of whatever that male was pumping (or saying he was pumping). To be honest, I think the whole paper is an AGP fantasy, but that it was published and what was described didn’t raise any formal child protection bells greatly concerns me.
LikeLiked by 1 person
Reblogged this on vaskaxtumir and commented:
“On presentation, the patient was on a gender-affirming regimen that included spironolactone (a heart medication used in this case as an androgen blocker), estradiol, micronised progesterone and “occasional” clonazepam and zolpidem for panic disorder and insomnia.”
LikeLiked by 1 person
Why are you not on Facebook? Many Radical Feminists groups are on FB and I get their articles everyday but with this blog I only get articles if other groups post to their sites. I would love to see your work on a regular basis.
Great article. Truly frightening this frankenstein manipulation of healthy human bodies and the experimentation on children. I recommend, in case you are not already familiar with her, the “idge of reason”, a You Tube channel.. She talks about having been a social worker in the UK for a decade and the transgender activism actively moving towards the legalization of pedophilia of course, along with other pedophiles who have never really been able to accomplish this due to, as you say, the social unacceptability of pedophilia however, with the trans lobby everything is becoming acceptable through their activism being framed as transphobic if anyone argues against anything they desire.
LikeLike
Dear Laurie, thank you for your comment! The reason I’m not on facebook is because the abuse by trans activists is very stressful and unfortunately, my chronic health condition forces me to avoid stress, or my asthma gets badly triggered and I’m out of action for months. I wish I didn’t have that limitation, but can’t really do much about it.
I know Lisa Muggeridge and miss her greatly on twitter! Her contribution has been an eye opener for many of us. I also have long suspected paedophile activism is behind all this, certainly it is fundamental to queer theory which has spawned this ideology, and the fathers of gender reassignment intervention itself were all campaigning to lower or abolish age of consent (Kinsey, Money, Benjamin). It’s an old monster in a new frock, and it’s unsurprising they have the ear of institutions – it’s always been the case. If you haven’t seen this before, Dr EM has analysed a Paedophile Manifesto on twitter, and the parallels with methods of transactivists speak for themselves. https://mobile.twitter.com/PankhurstEM/status/991258041038368768
LikeLiked by 1 person
You maintained a scientific appearance throughout, but some sources don’t look scientific to me.
Most notably, you claim “psychosexual disorders such as autogynaephilia are present…”. Yet no researcher has ever claimed that autogynaephilia is a psychosexual disorder, or a disorder at all. It was claimed as etiology for (what was then known as) gender identity disorder, but not as a disorder in its own right. Your quoted source is an activist website. But you allege an ethical issue specifically based on it being a “disorder”.
LikeLike
I have appraised a case study from a medical perspective, using my knowledge and references I deem fit in this context. Autogynaephilia is a paraphilia and as such is a psychosexual disorder. I’m not “maintaining an appearance” of anything. I’m offering my medical opinion.
LikeLiked by 3 people
Excellent informative piece that is rightly attentive to what was ignored in the original “trans identified male bravely realizes his dreams” account: the health of the child subjected to experimentation
LikeLiked by 2 people
Reblogged this on Madam Nomad and commented:
La Lecher League has been actively promoting male breastfeeding. Chemical Male Mothering, i.e., eugenic medical endocrine fuckery, is Frankensteinian ghoulishness.
LikeLike
I’m on your side on this, but it’s important that we remain careful and fact-based.
Paraphilias aren’t disorders. They can be, but not necessarily. Even Ray Blanchard has made this point.
IIRC, Blanchard said that a paraphilia becomes a disorder if it causes its haver distress, or causes him to harm others. Lactating for personal gratification while ignoring, or, at best, showing minimal concern for, a baby’s needs, would qualify.
LikeLike
Blanchard can have his opinion but from a psychiatric perspective paraphilias are psychosexual disorders.
LikeLiked by 3 people
This highly questionable (from the truth point of view) report of a biological male breastfeeding has surfaced (yet) again, being lauded by the Milk Meg, who has run a Facebook page for years, supporting women all over the world with normally great knowledge and warmth. Her followers are thrilled too and even questioning posts are being deleted. It’s very sad that in the desire to be open minded and supportive of breastfeeding, Meg and her followers don’t see the inconsistencies and seem blind to the big question ‘why is someone making this stuff up’? I wonder if they’ve ever heard of ‘lactation porn’? (Only one of many possible elements in this).
LikeLiked by 1 person
Unfortunately many women, and especially ambitious ones, are eager to virtue signal to men and the trans lobby. As a feminist I often wonder why this is so, and despair at lack of sisterhood and self-sabotage that seems inherent in female society. Women as a class are mostly unaware and in denial about patriarchy and oppression, and their reflex is to mollify and exalt men at all costs. We are violently socialised to be this way, nevertheless, it’s infuriating because this women policing and ostracising women who aren’t as eager to service men’s needs constitutes a betrayal that keeps our communities fractured and our liberation from male oppression out of reach. It’s all very tragic and disappointing. Still, we must persist and not lose hope. xx
LikeLiked by 2 people
I am glad to see people breaking it down and calling it out. This shit has been creeping it’s way through all of society for far too long. I hope once more catch on to the child abuse they will realize that this is very much to serve super rich men with all kinds of perversions.
After reading this “study” it was so obvious there was much wrong that needed to be questioned. We have to stop this madness!
LikeLiked by 1 person
This is truly excellent and I am delighted to see it. Given the media rewards for being the “first” to do anything controversial, you are right to point out that it would be good to see some proof of breastfeeding. As for the meds: I think of the crazy concerns about women taking something for cold, or having a glass of wine,or trace pesticide residue…… yet if it is a man…
LikeLiked by 2 people
I looked into all the claims I have seen of men “breastfeeding” over the years and none stand up to scrutiny not to mention half are just plain fictional stories.
When I read this study it said the males milk was similar to that of colostrum…pishhh…let me see those lab results.🙄
LikeLiked by 2 people
Im sitting here typing out what I want to say, erasing it, and typing out more words…but..this is child abuse in my opinion. It actually reduced me to tears.
LikeLiked by 1 person
I know how you feel. I was shocked and appalled that this was even written up, in my opinion it is fiction and designed to promote an unethical practice. It was uncritically reported in news outlets and it led to many breastfeeding charities jumping on the gender ideology bandwagon, which was shocking to watch. It demonstrated how unfit so many people in charge of women’s orgs are.
LikeLiked by 1 person
The fact that you would risk so much to stand up for other women, and for children is inspiring. I can only hope that you are correct, and that it is fiction. Can I ask, would a male emmission that passes for milk expressed from a male breast, even be nutritious for a baby? I resent even wondering that question, my friend. How on earth can something as solely female as breastfeeding be hijacked. It is clearly being used as a kink. I saw a blog on here posting an ‘erotic’ style story regarding breastfeeding. I wish I had bookmarked it to show you, but was so horrified I just pressed block immediately. Rape crisis in my area has been hijacked by men – I had a man answer the phone, and refuse to pass me to a female. Shelters are all mixed, there is not one single SEX shelter, not even a DV one. Not fit for purpose!
LikeLiked by 1 person
Men taking over services for abused and vulnerable women has one goal only and it is not a good one. This is what women and feminists have been fighting ever since men burned down the first women-only public toilet. All female physiological functions are a fetish to some men, and this is the safeguarding concern inherent in these policies.
To answer your question, male nipple discharge is always pathological and mostly water. There are historical records of men “breastfeeding” infants on long boat journeys because mother has died. It was seen as inadequate but it provided mostly fluids and may have saved a child’s life. But these reports are anecdotal. Medically we know men who have nipple discharge either have certain endocrine tumours causing excess prolactin, or this can also happen as a side effect of medication. It doesn’t contain most beneficial substances that mother’s milk provides (especially early on), but it has potential toxins. There is no way to make this kind of thing ethical, not if you consider interests of the child.
LikeLiked by 1 person
That is disgustingly fascinating! Surely the medical profession cannot allow a man to feed this discharge to a baby? I know nothing of ethics, but turning a baby into a sexual validation prop at the expense of the baby’s health surely is totally unethical.
As for the safeguarding aspect, I wish I could come and give you a huge pat on the back. I have been shouted down by women who provide shelter services, these women telling me “trans women are woman” in their handmaiden frenzied way, and that really made getting into a shelter very difficult for me indeed. It isn’t just me who now doesn’t drink all morning if I have to go out – in SF public bathrooms are not an option.
They always say that history won’t be on our side. I personally think history will see you are the good doctor who would not be bowed under pressure and stood her ground for what was right.
LikeLiked by 1 person
I’m so sorry that you have to deal with handmaidens, this is a real problem here in the UK and as always, women who are vulnerable – homeless, fleeing violence, sick, disabled – are the ones put in danger while those who have no such vulnerabilities are selling out the rest down the river for male approval and funding.
LikeLiked by 1 person
That is exactly right – it is an issue of being privileged enough to be ‘woke’. The rest of us are down here in reality. Thank you for speaking up, la scapigliata, It is always a pleasure to hear from you.
LikeLiked by 1 person